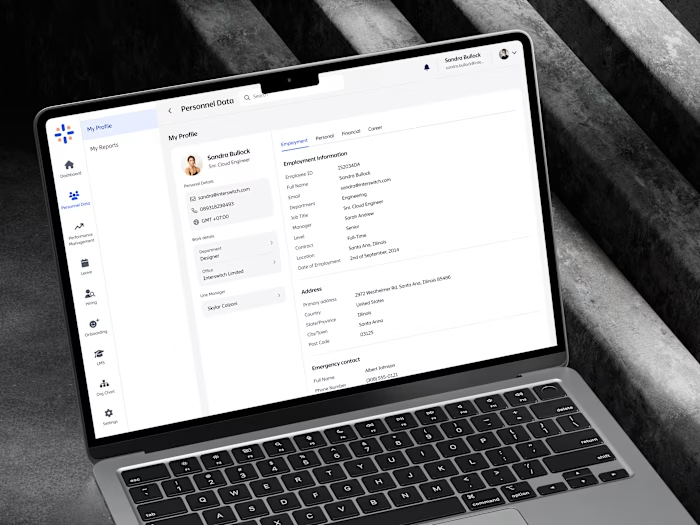
Claims Automation: Reliance Health
Insurance Automation: 48% Faster Claims, 23% Lower Costs
The Problem
Reliance Health's claims processing system was almost entirely manual, requiring human review for every single claim. This created a perfect storm of problems: human errors led to incorrect approvals and denials, fraudulent claims slipped through because reviewers couldn't catch patterns, processing times were painfully slow (averaging 7-10 days), and the medical expense ratio was climbing as costs outpaced premiums.
With hundreds of thousands of members filing claims, the manual system couldn't scale. Every delayed or incorrect claim damaged member trust and corporate client relationships.
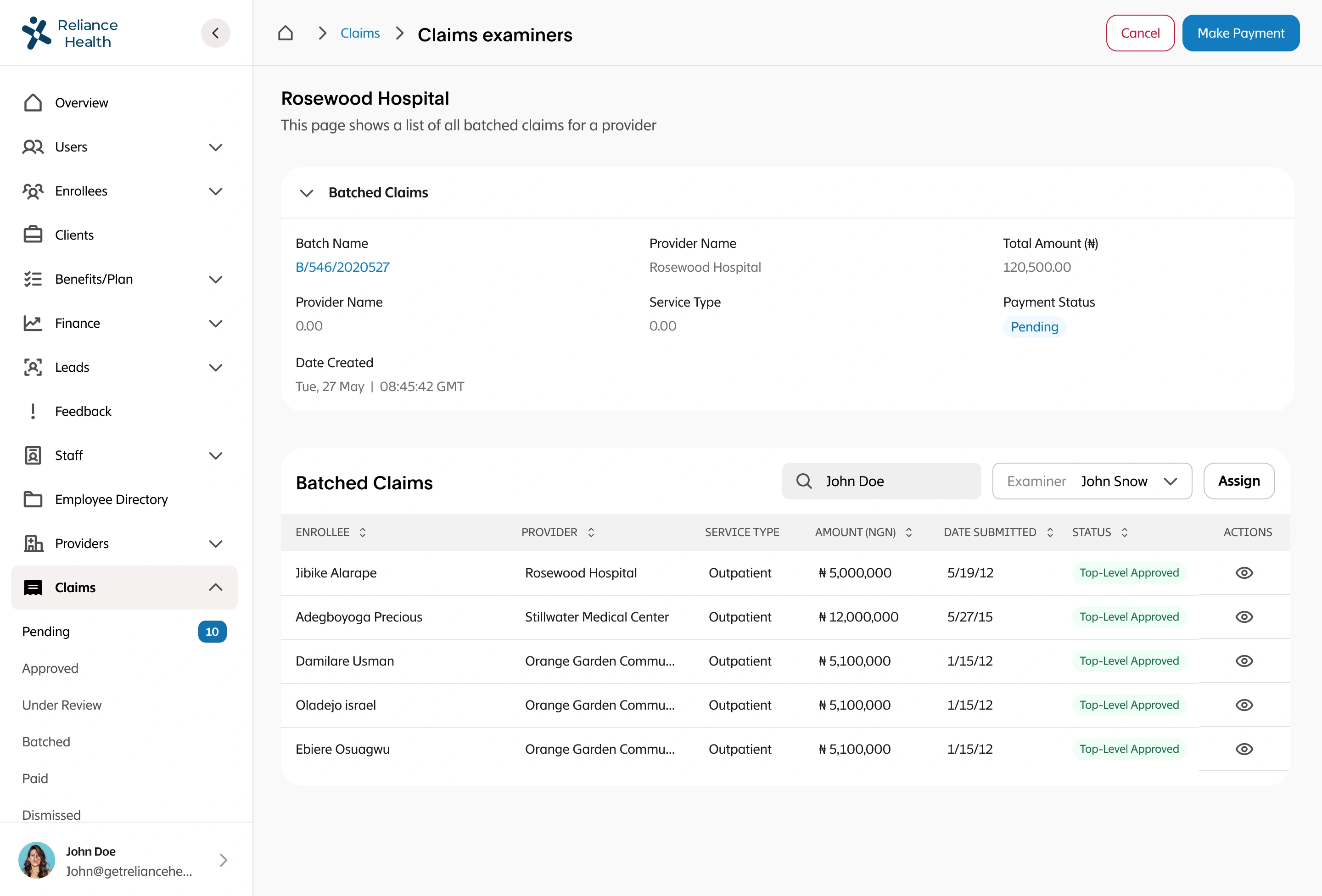
What I Did
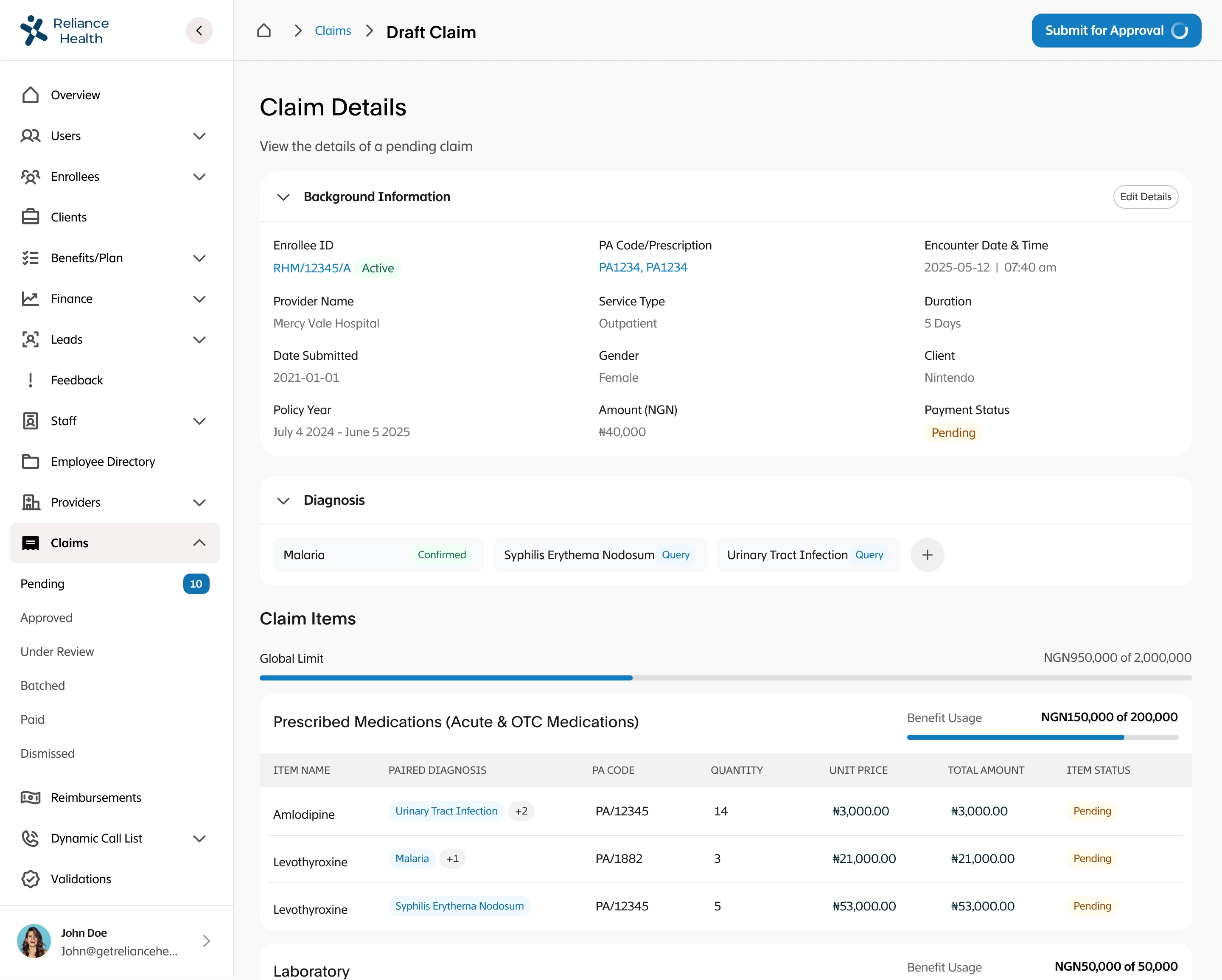
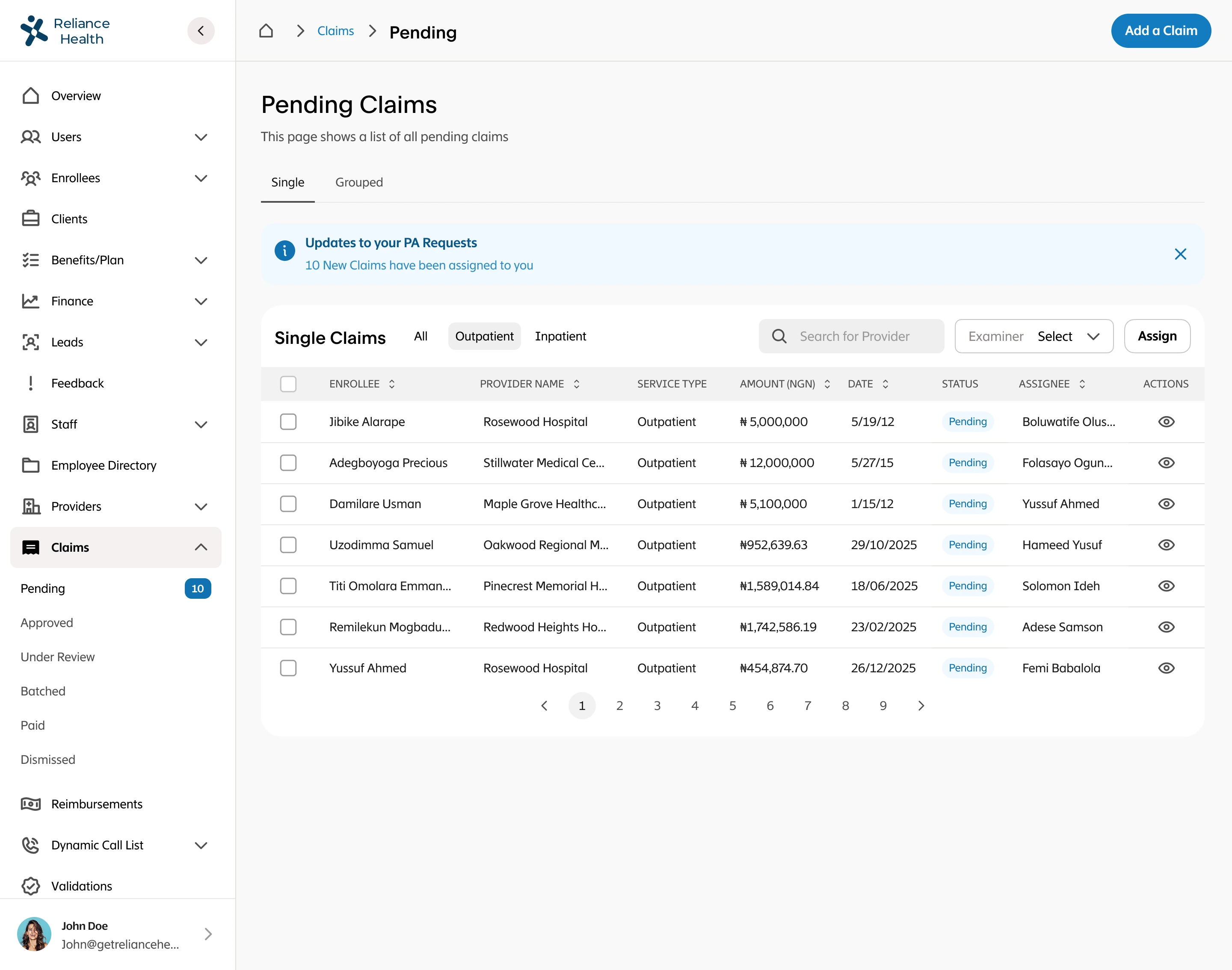
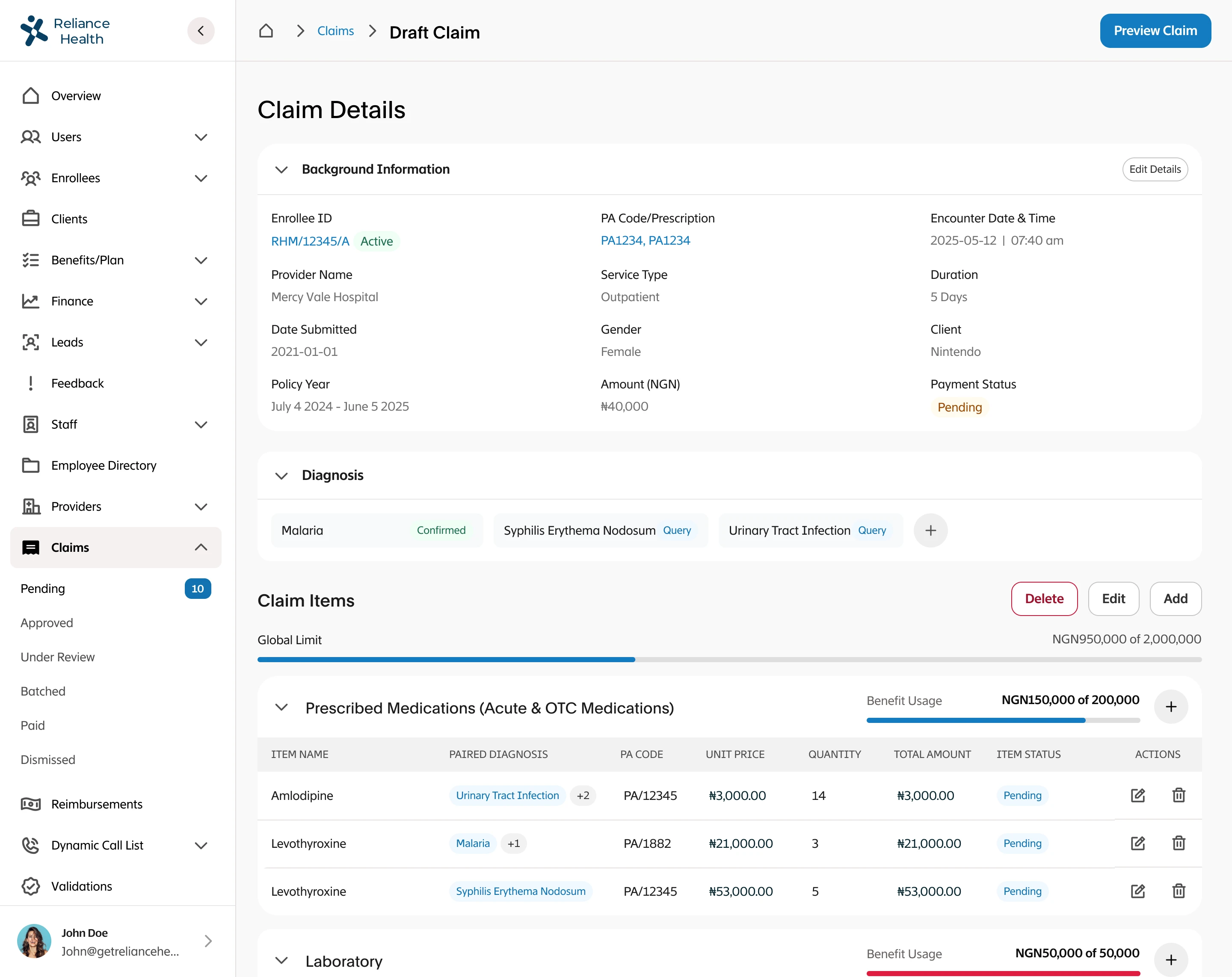
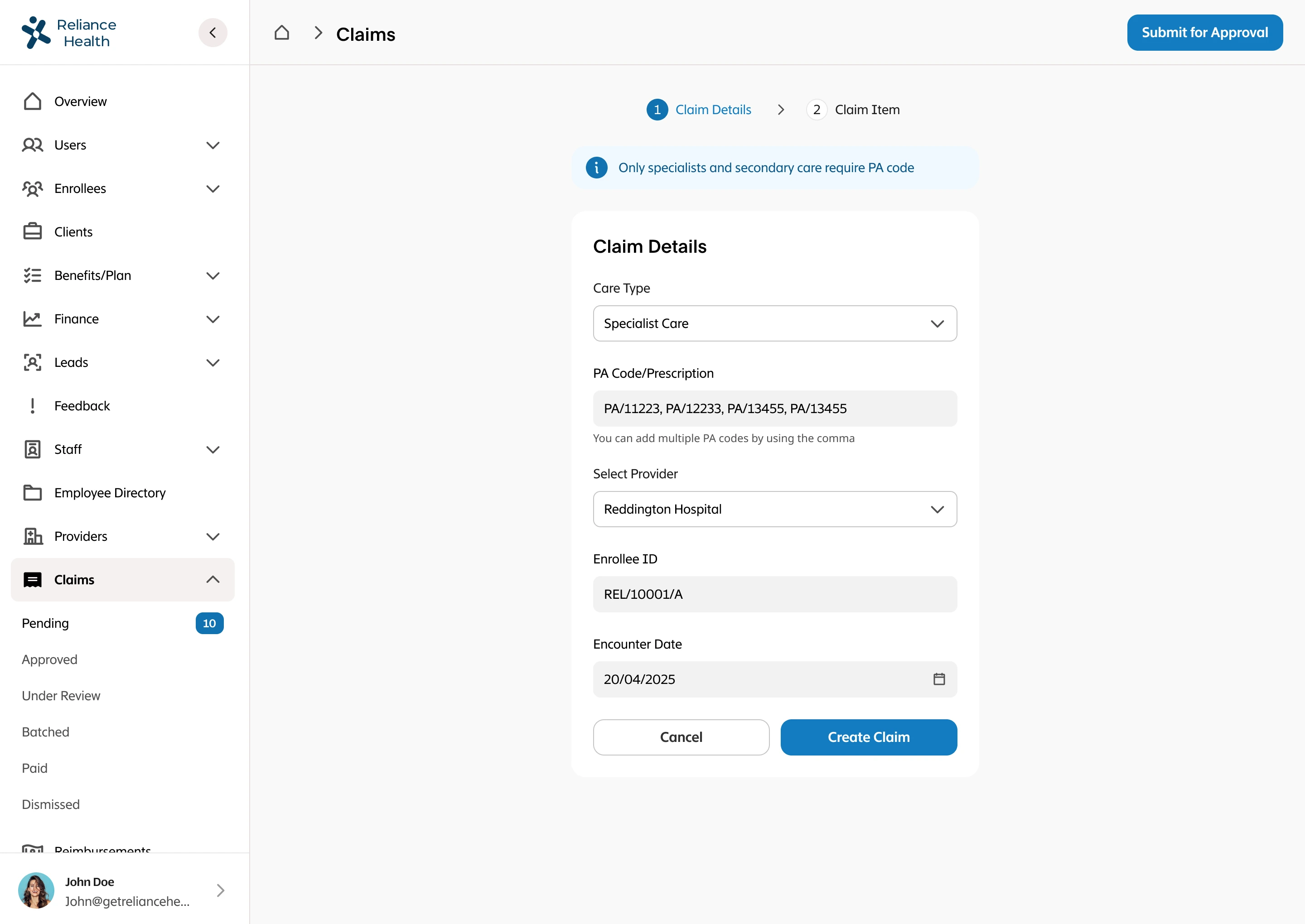
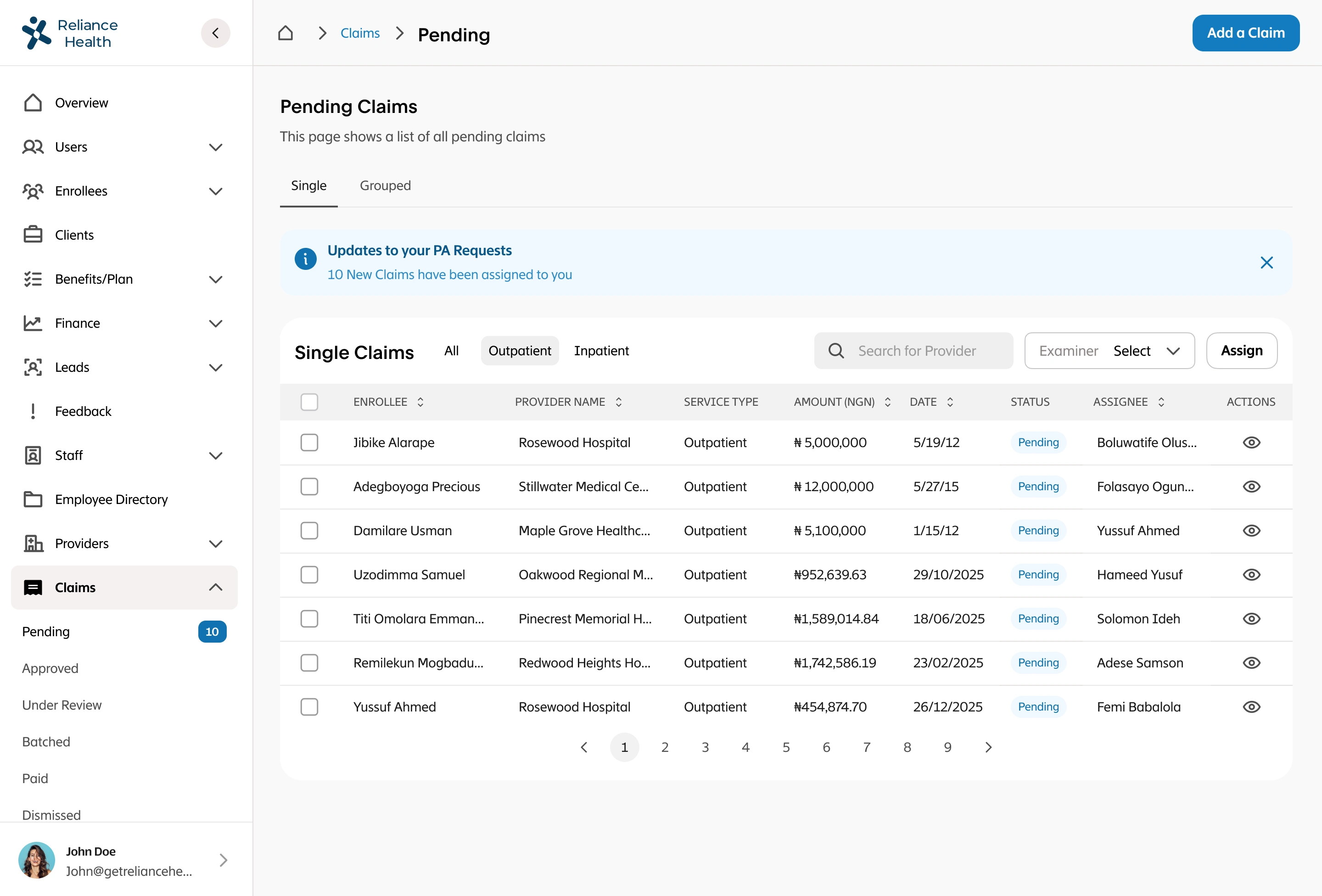
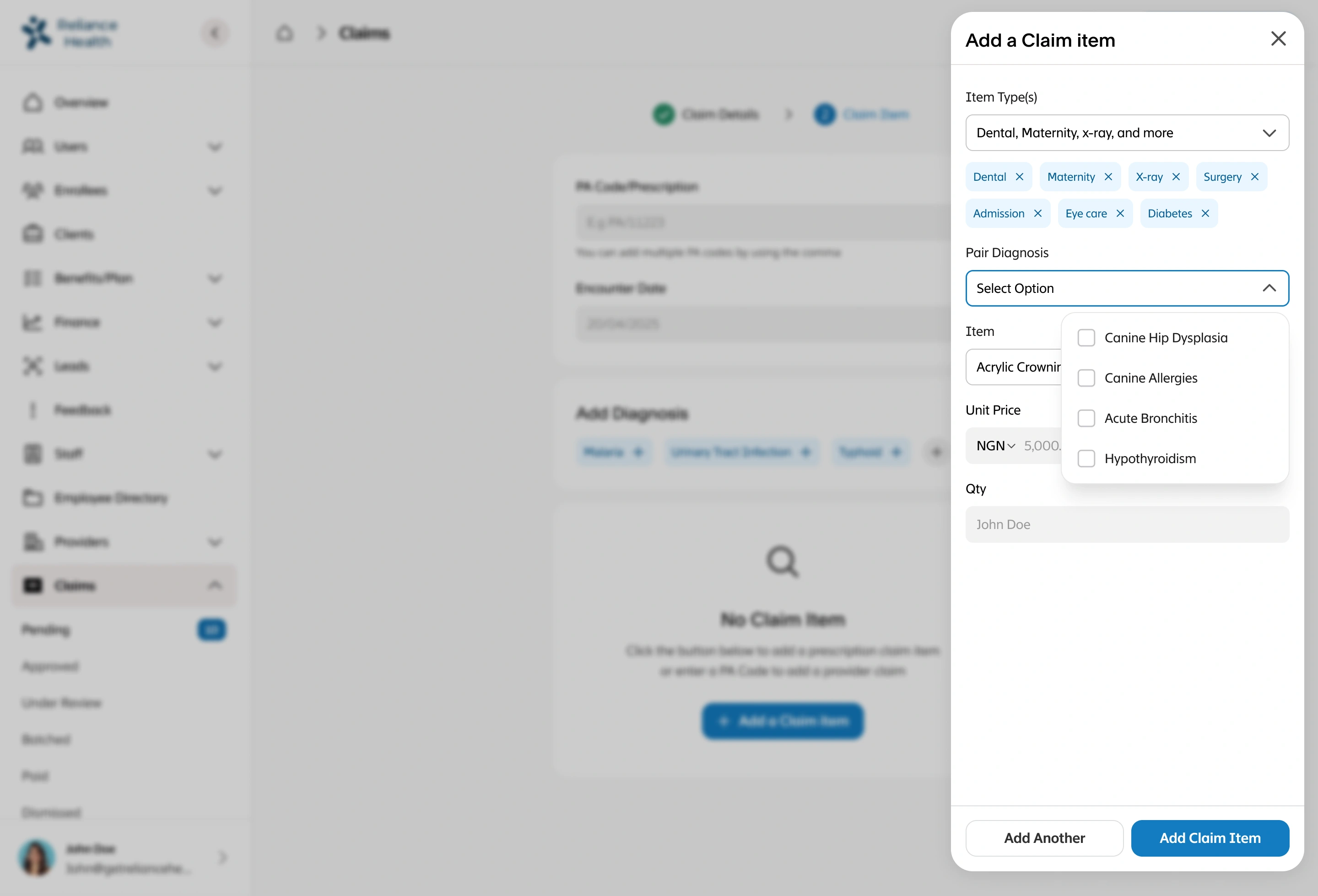
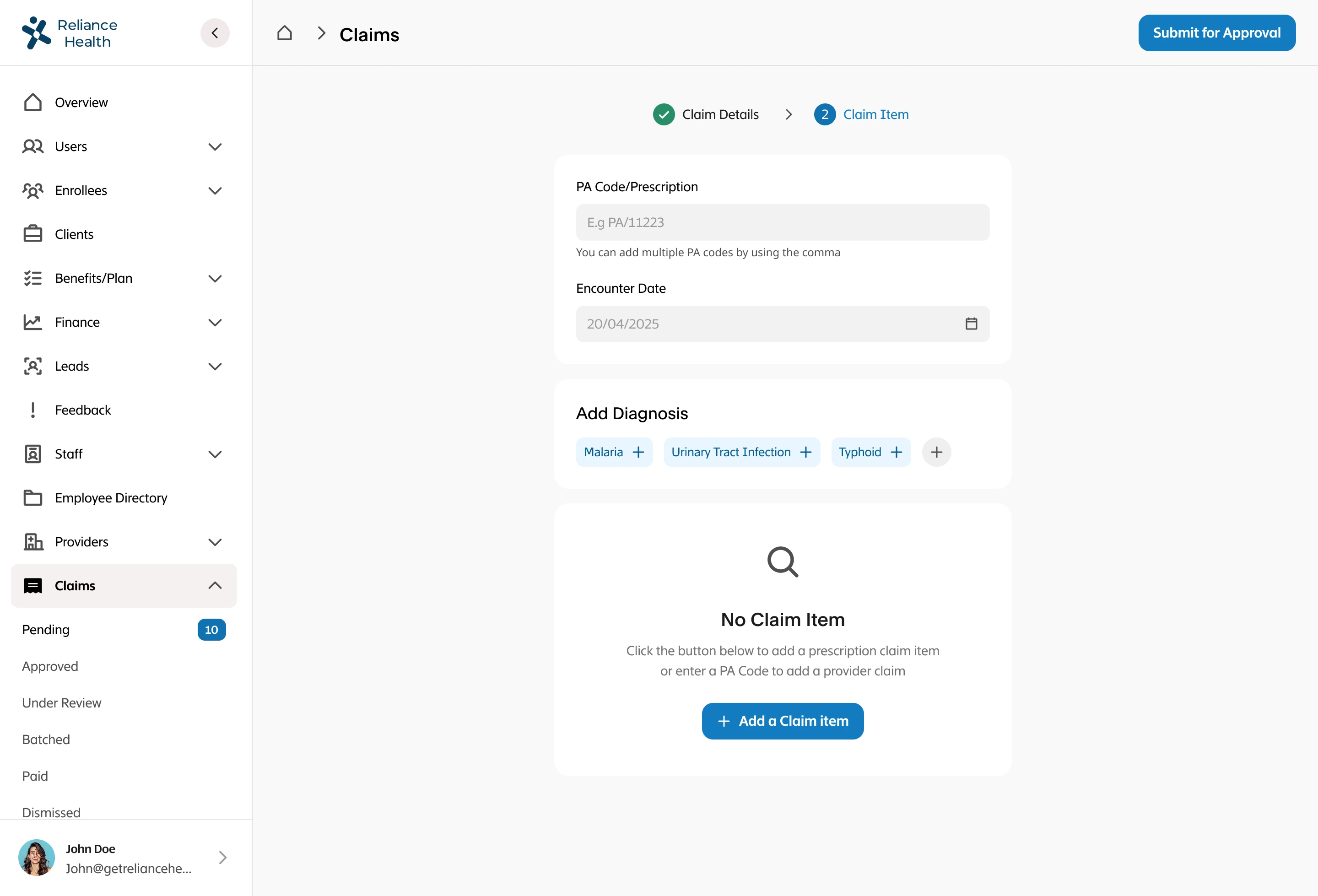
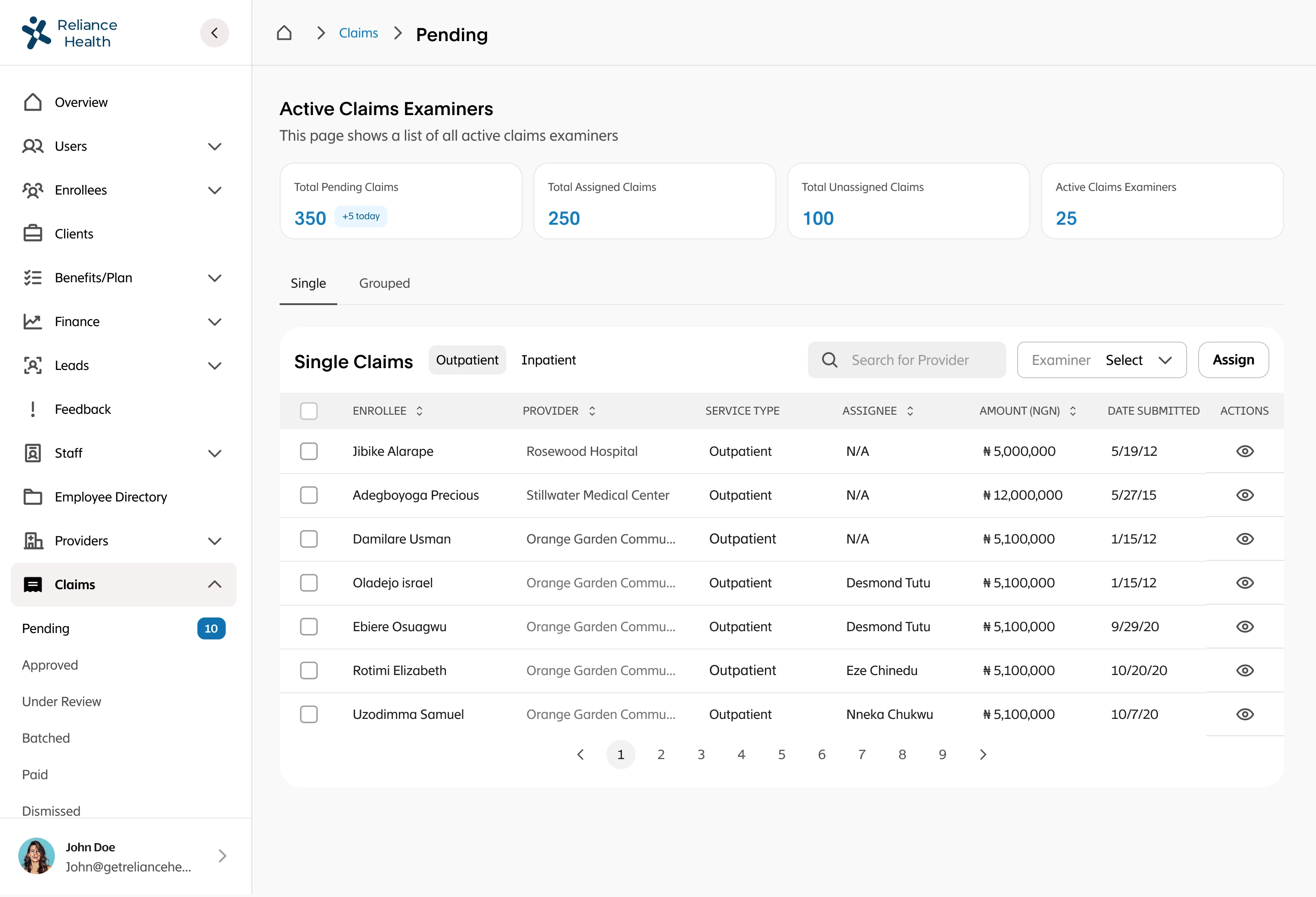
I led the complete redesign of the claims processing workflow, integrating automation to reduce human intervention to only exceptional cases. I designed intelligent fraud detection workflows that flagged suspicious patterns, created automated validation rules based on policy terms and medical standards, built exception handling for edge cases that required human judgment, designed real-time status tracking for members and providers, and created dashboards for claims adjusters to quickly review only the cases that needed human attention. The system had to balance speed with accuracy while maintaining compliance with insurance regulations.
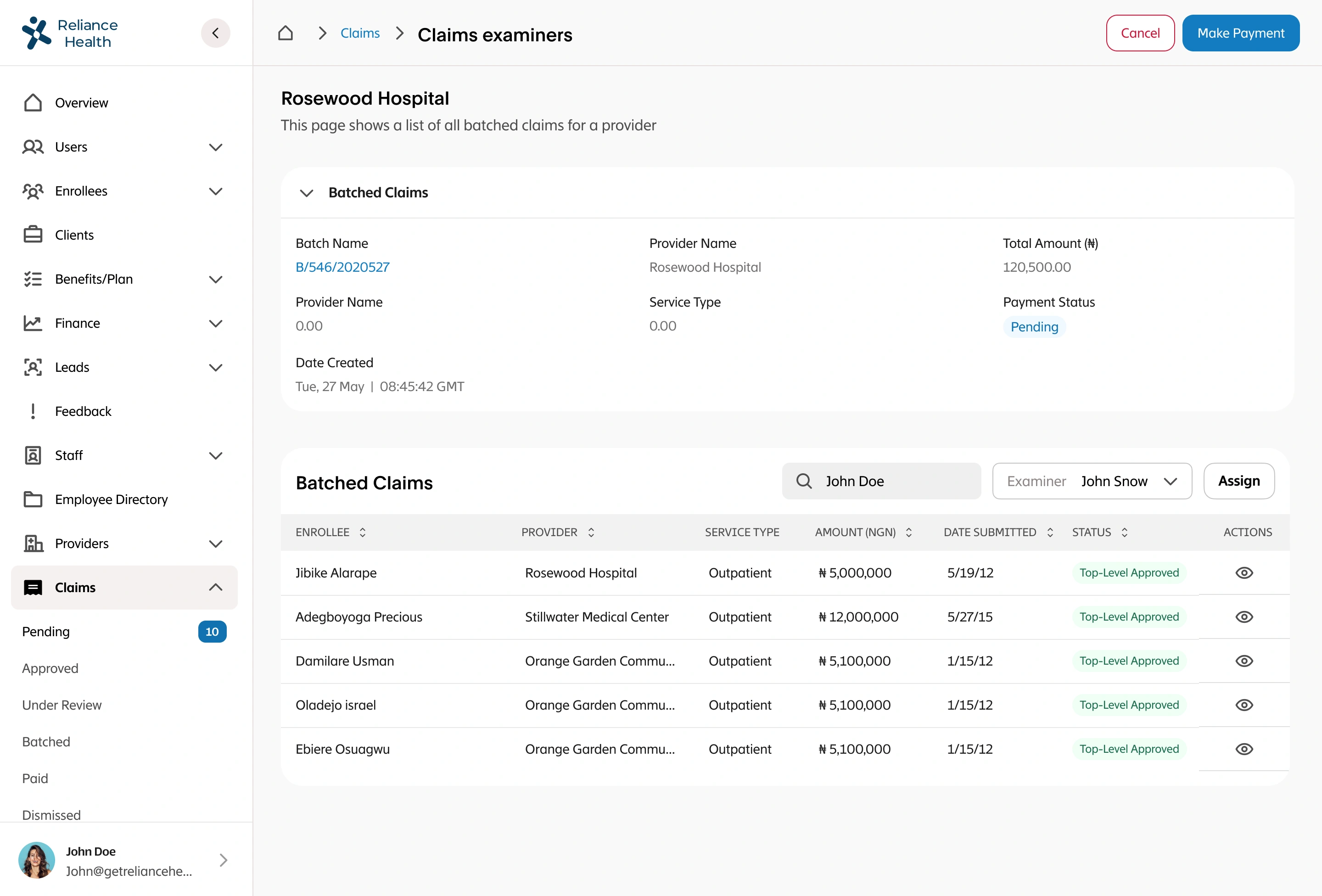
Where It Got Messy
Halfway through implementation, we realized our fraud detection algorithm was flagging legitimate claims from rural areas as suspicious because rural healthcare costs looked statistically different from urban patterns. We were about to deny thousands of valid claims from some of Nigeria's most underserved communities.
I had to completely redesign the fraud detection logic to account for geographic healthcare cost variations, work with the data science team to retrain the models, and add manual override capabilities for claims adjusters who understood regional
patterns. It delayed our launch by 6 weeks and required sensitive internal
conversations about algorithmic bias.
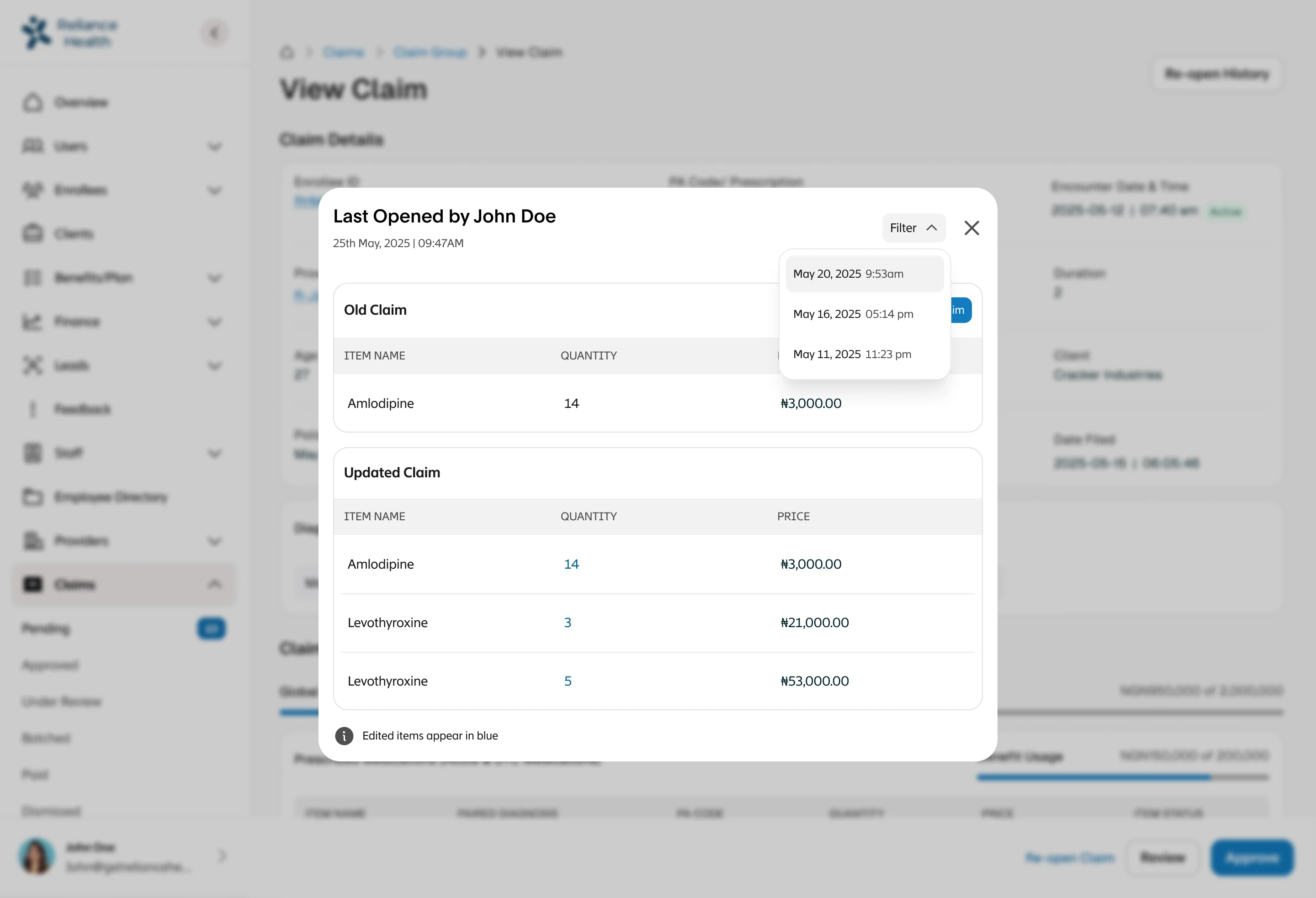
Results
Claims processing speed increased 48% within 4 months. NPS score jumped from 45% to 63% as members got faster responses. Human error rate decreased 64% due to automation. Medical expense ratio decreased 23%, saving millions annually in operational costs.
Fraud detection caught patterns human reviewers had missed, preventing estimated $2M+ in fraudulent payouts. Corporate client retention improved because claims processing became a competitive advantage instead of a weakness.
Like this project
Posted Apr 22, 2026
Redesigned Reliance Health's claims processing with automation, reducing errors and improving speed.
Likes
1
Views
2
Timeline
Feb 17, 2025 - Jun 27, 2025
Clients
Reliance Health
Collaborators