Ana Paola Morales
Biomedical engineer for technical research & documentation
New to Contra
Ana Paola is ready for their next project!
Exercise as protection in older age
A persistent myth suggests older adults should avoid exercise to prevent injury. Evidence shows the opposite. Explaining strength training as safe when properly prescribed. Large reviews in adults over 60—and even over 80—report that serious exercise-related events are rare, with most issues limited to temporary muscle or joint soreness. Risk increases primarily with poor technique, excessive intensity, or inadequate progression. When exercise is adapted, supervised, and progressed gradually, it becomes protective: reducing falls, preserving independence, and counteracting age-related decline. Inactivity, not movement, is the greater risk.
17
91
Disability access: progress in policy, limits in practice
Accessibility for people with disabilities has improved on paper, but research shows a persistent gap between law and daily life. Many countries have strong legal frameworks, yet enforcement remains weak. Studies report widespread barriers in streets, public buildings, and transport—uneven paths, missing ramps or lifts, narrow doors, and inaccessible toilets. These obstacles reduce safety, independence, access to work, education, healthcare, and social participation. Evidence consistently shows that, especially in low- and middle-income contexts, accessibility is still far from adequate for most people with disabilities.
17
91
Why a suitable wheelchair matters
A wheelchair is not just a mobility aid—it is essential for health, independence, and participation. Poorly fitted or generic chairs can cause pain, postural deformities, and pressure injuries, while appropriate seating improves comfort, stability, and safety. Proper fit and posture support also affect bladder management and prevention of secondary complications. Beyond health, suitable wheelchairs enable mobility, work, education, and social life. International frameworks recognize access to an appropriate wheelchair as a human right, not a luxury.
12
66
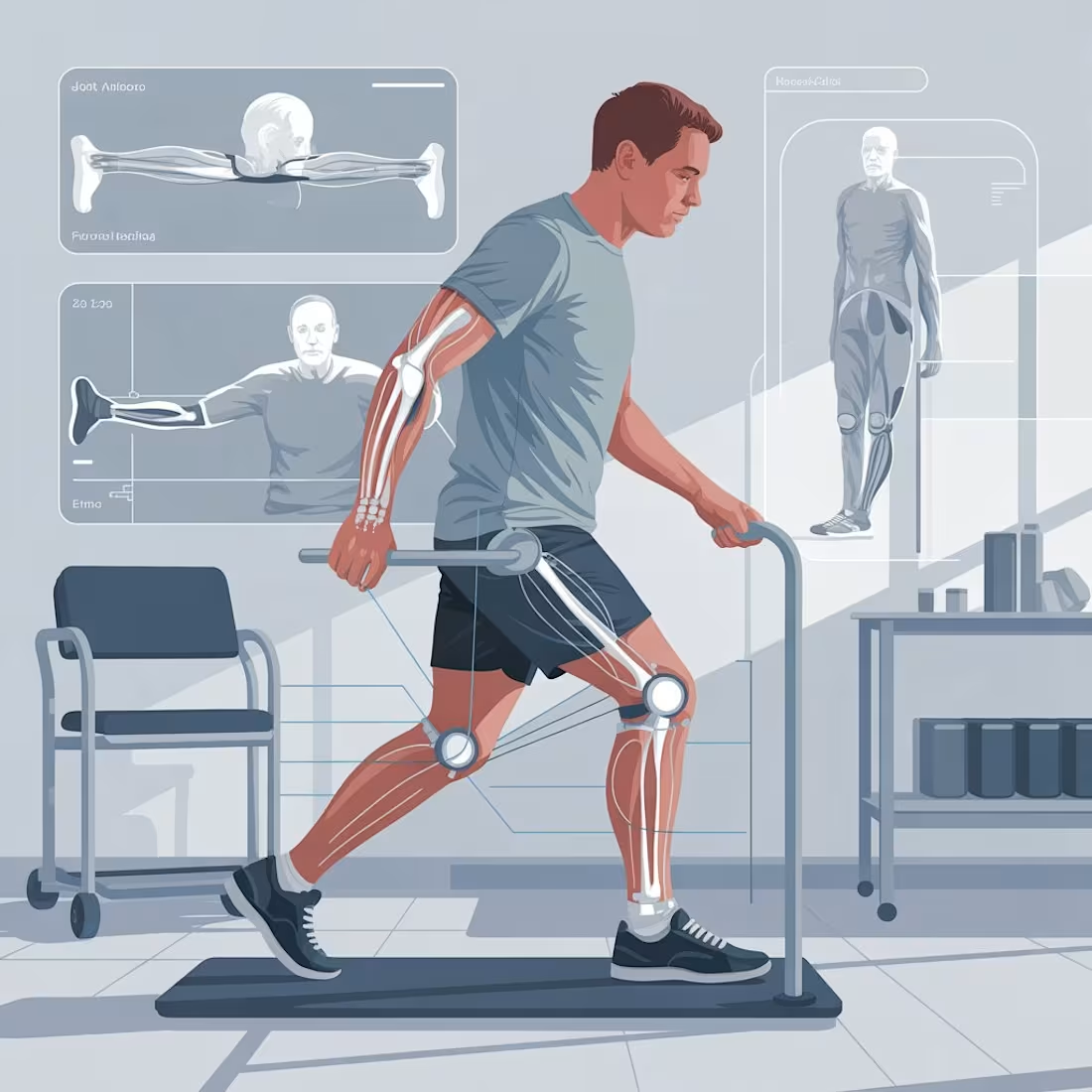
Biomechanics in rehabilitation: from movement data to better recovery
Biomechanics helps rehabilitation by objectively measuring how people with disabilities move and interact with forces. Tools such as motion capture, force plates, and EMG quantify gait, joint motion, muscle activation, and balance, allowing clinicians to identify impairments and compensations. These data support personalized therapy, track recovery more accurately than clinical scales, and inform the design of assistive technologies such as orthoses, prostheses, and exoskeletons. Biomechanics does not replace therapists, but strengthens rehabilitation by making decisions more precise, adaptive, and evidence-based.
0
10